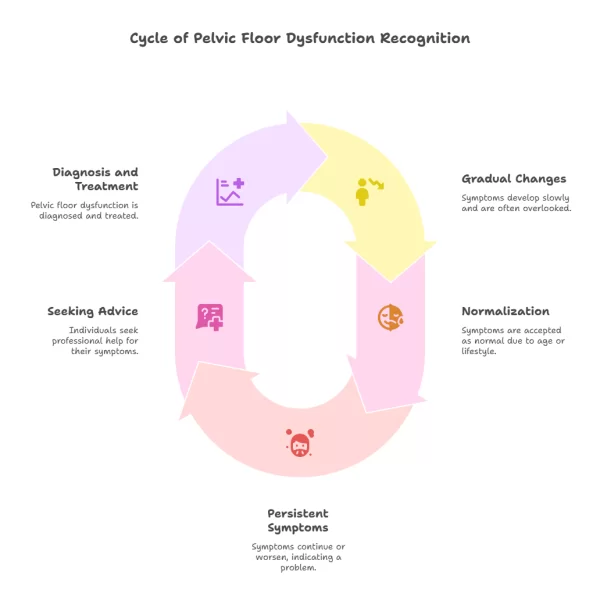
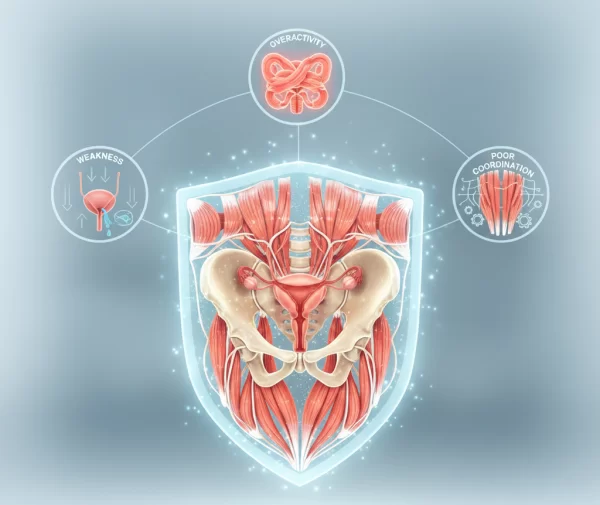
Pelvic floor dysfunction can present in several different ways, depending on how the muscles are affected. While symptoms often overlap, clinicians generally group pelvic floor problems into a small number of patterns to guide assessment and treatment.
Pelvic floor weakness
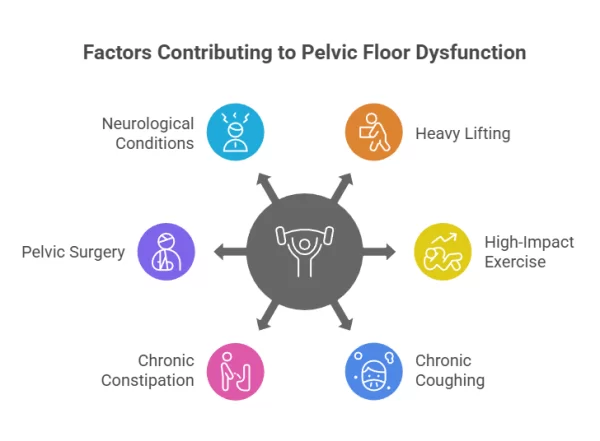
Pelvic floor weakness occurs when the muscles are unable to provide adequate support or control. This is commonly associated with pregnancy, childbirth, menopause, pelvic surgery, or long-term strain.
Key features often include:
-
Leakage of urine during activities such as coughing, laughing, or exercise.
-
A feeling of heaviness or pressure in the pelvis.
-
Reduced control over bladder or bowel function.
Although weakness is a frequent cause of leakage, it is not the only one. This is why exercises alone are not always the right starting point without proper assessment.
Overactive or tight pelvic floor muscles
In some people, the pelvic floor muscles are overly tense and have difficulty relaxing. This pattern is sometimes overlooked because it can exist alongside symptoms that resemble weakness.
Common features may include:
-
Pelvic pain or discomfort.
-
Pain during intimacy.
-
Difficulty fully emptying the bladder or bowel.
-
Urgency or leakage is linked to poor muscle coordination rather than a lack of strength.
In these cases, strengthening exercises without guidance can worsen symptoms, making an accurate diagnosis particularly important.
Pelvic organ prolapse
Pelvic organ prolapse occurs when one or more pelvic organs move downwards due to reduced support. The degree of prolapse varies widely and does not always correlate with symptom severity.
People may notice:
-
A sensation of dragging or fullness.
-
A visible or palpable bulge.
-
Changes in bladder or bowel habits.
Many cases are mild and managed conservatively. Surgery is not always required, and treatment decisions are based on symptoms, impact on daily life, and individual preference.
Pelvic floor dysfunction is not a single condition, but a group of related patterns with different causes and management approaches. Recognising these distinctions helps avoid assumptions and supports more effective care.